Laser Therapy for Pain & Inflammation
1064 nm Photobiomodulation (PBM)
Non-thermal light therapy designed to support tissue recovery, regulate inflammation, and promote cellular repair.
Medical-grade photobiomodulation systems. Protocol-driven care. Functional outcomes.
How PBM therapy supports healing
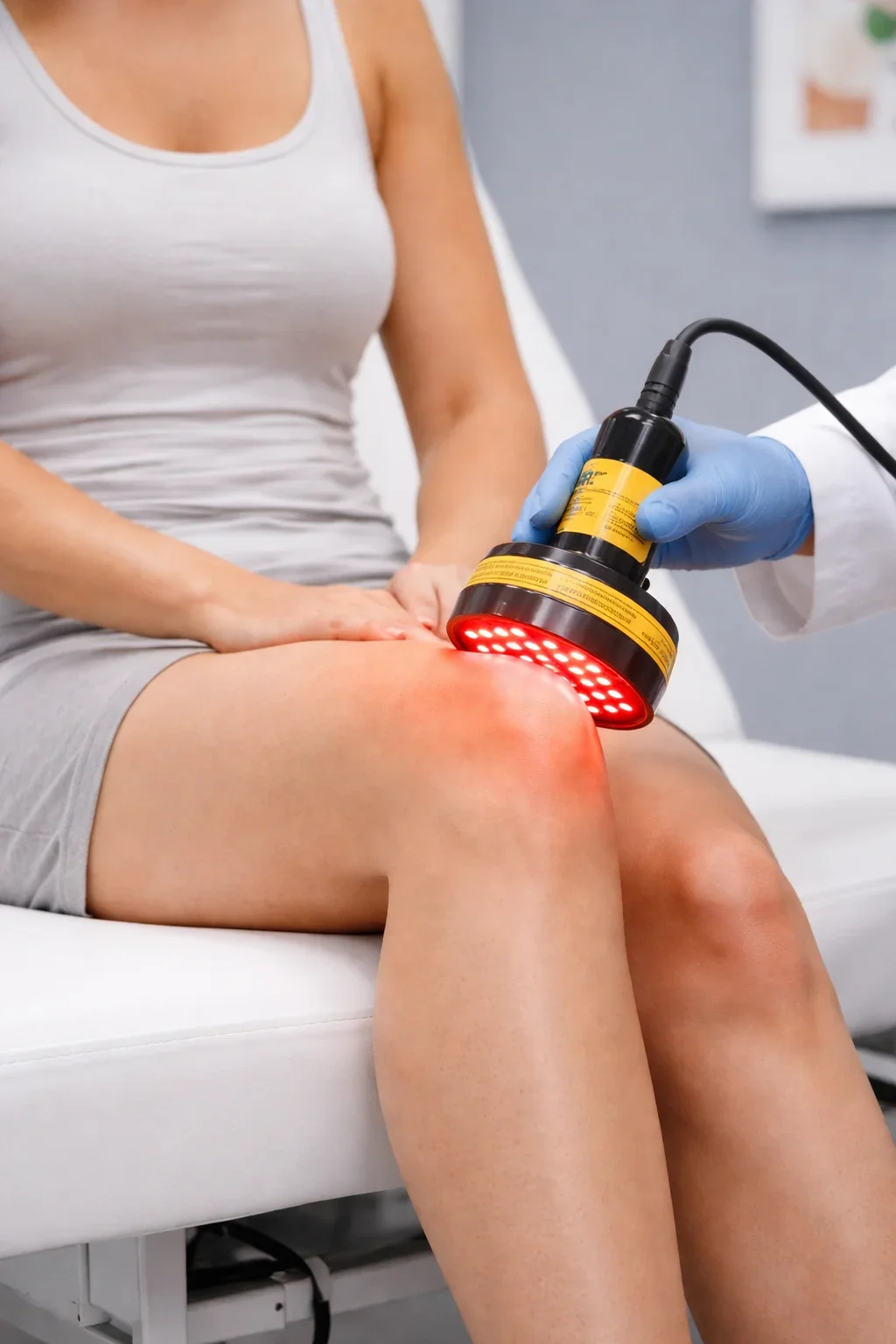
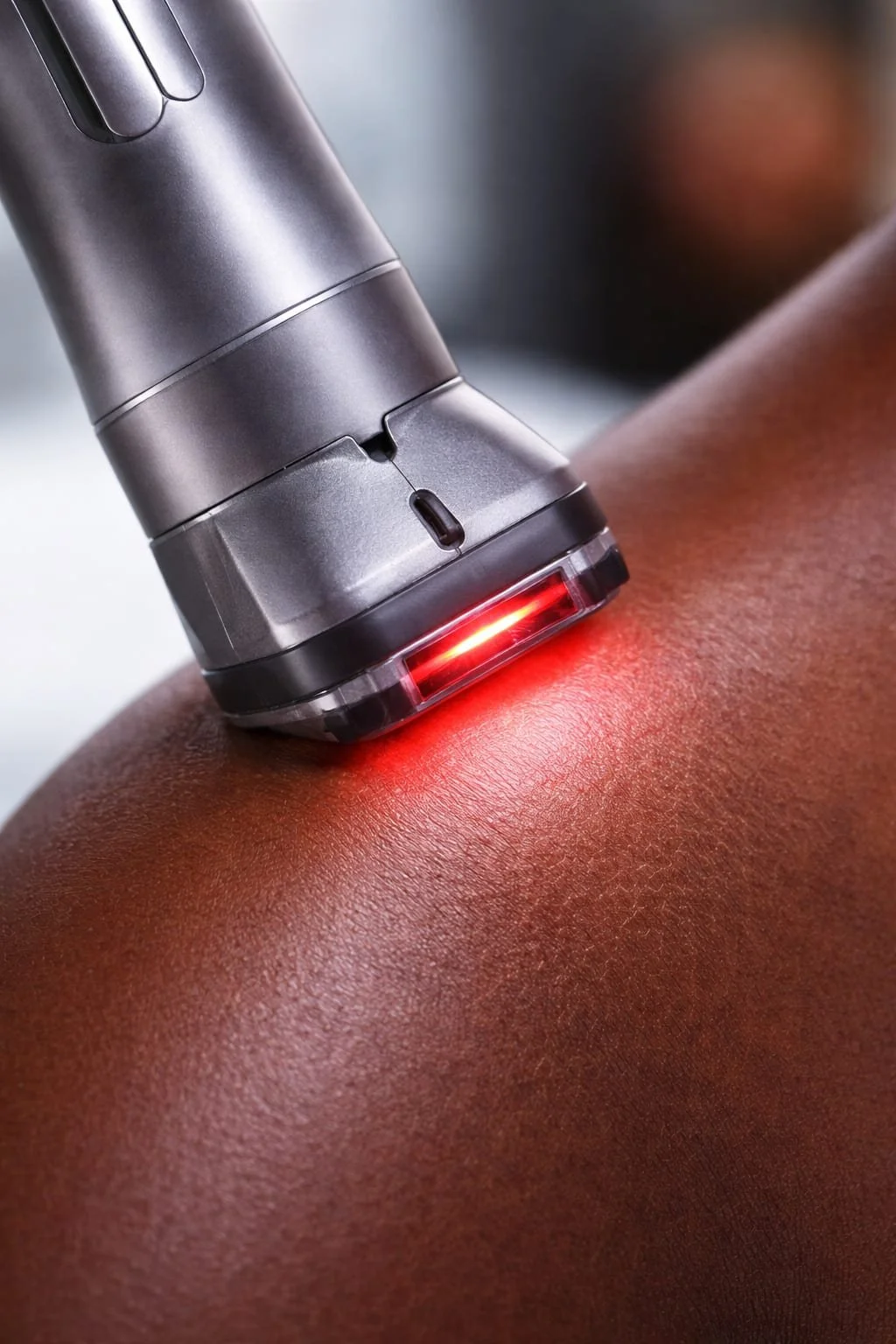
Photobiomodulation therapy delivers non-thermal light energy to targeted tissue to support cellular function and recovery.
Energy is absorbed at a cellular level, supporting improved microcirculation, modulation of inflammatory mediators, and optimized tissue repair processes.
Clinically, PBM is used to support recovery in muscle, connective tissue, nerve pathways, and post-procedural skin healing. It may be delivered as a primary treatment for pain and inflammation or as an adjunct to laser procedures to enhance recovery timelines.
What PBM therapy is used for
Photobiomodulation therapy is commonly used to support recovery in musculoskeletal pain and soft-tissue injuries, joint inflammation and overuse syndromes, and myofascial trigger point disorders.
It may also assist with peripheral nerve irritation, post-surgical or post-procedural tissue recovery, scar management and connective tissue remodelling, and functional recovery related to physical strain or performance demands.
Common Clinical Presentations
Tendinopathies (Achilles, patellar, rotator cuff)
Rotator cuff and shoulder irritation
Plantar fasciitis
Lumbar strain and paraspinal muscle injury
Lateral or medial epicondylitis (tennis or golfer’s elbow)
Myofascial pain syndrome
Peripheral nerve irritation
Post-surgical inflammation and swelling
Patients may seek PBM therapy directly or be referred by physicians, physiotherapists, and other healthcare providers for adjunctive support in cases involving tissue recovery, inflammation modulation, post-procedural healing, or chronic musculoskeletal pain.
A clinical, response-based approach
Photobiomodulation therapy at LaserLite Solutions is delivered using structured, indication-specific protocols. Treatment parameters are selected based on tissue type, anatomical location, and clinical presentation.
Session duration, treatment frequency, and progression are guided by observed tissue response and functional outcomes rather than fixed timelines.
Parameters are adjusted according to objective clinical response and tissue tolerance. PBM may be delivered as a standalone therapeutic intervention or integrated into a broader laser or recovery plan when clinically appropriate.
Clear expectations
Photobiomodulation therapy is not a cosmetic intervention and does not produce immediate aesthetic change. Clinical effects develop progressively as tissue responds at the cellular level.
PBM is not a replacement for medical diagnosis, emergency care, or specialist management. It is delivered as a structured, evidence-informed therapeutic intervention to support tissue recovery, inflammation modulation, and functional improvement.
Individual response varies based on tissue condition, severity, and adherence to recommended treatment frequency.
Who this therapy may benefit
Photobiomodulation therapy is appropriate for individuals seeking non-invasive, clinically guided support for pain modulation, inflammation control, post-injury recovery, and tissue healing.
It is commonly incorporated into care plans for chronic musculoskeletal conditions, post-surgical rehabilitation, nerve-related discomfort, overuse injuries, and performance recovery.
Protocols can be delivered across all skin types and anatomical regions. Treatment selection, dosing, and progression are determined by tissue response, clinical findings, and functional goals.
Assessment before treatment
All PBM services begin with a consultation to evaluate treatment goals, tissue characteristics, and clinical history. This ensures that therapy is appropriate and integrated into a clear care plan before sessions begin.